Medical Billing Vs Medical Coding - What's the Difference?
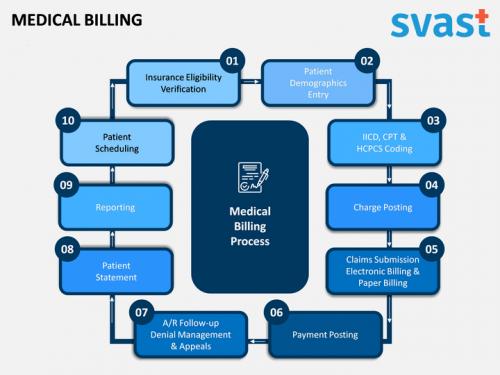
Medical
billing is an essential payment process within the United States
healthcare system. The process involves a health care provider submitting
claims for services rendered to the insured, following up with healthcare
insurance companies so as to obtain payment for medical services rendered;
including diagnostic tests, procedures, and treatments. The claims process is
usually managed by a claims specialist who has received specialized training in
medical billing and coding.
Medical billing
and coding outsourcing are a preferred choice of many providers because it
allows them to seamlessly integrate all areas of the business, from claims and
reimbursement to procurement and auditing. Medical billing outsourcing enables
service providers to quickly and easily submit claims to different healthcare
insurers. Some claim specialists also perform revenue cycle management tasks
that include scheduling of patients, maintaining patient records, and analyzing
billing information.
While an
in-house health insurance billing and coding specialist typically provide
medical billers and coders with comprehensive training in the medical billing
and coding process, there are instances where he or she may not be familiar
with specific areas. If this occurs, the provider can rely on an outside
service provider who is well-versed in all areas of the healthcare industry to
submit claims and/or code bills according to state laws, regulations, codes,
policies, and reimbursement options. A medical biller or coder can communicate
with the health insurance company and health insurer's claims adjuster
effectively and efficiently through electronic communication, allowing both
parties to meet their legal obligations.
A
professional Medical
billing and coding coder will generally have strong IT skills and
expertise in a wide variety of computer software programs and hardware, as well
as familiarity with payroll systems, accounting procedures, health insurance
forms, health care providers' software, health care insurance forms, patient
education, reimbursement processing, insurance claims processing, and billing.
An on-site medical coder can also assist with administrative tasks such as
filing insurance forms, assisting in the preparation of medical documents, and
answering phone calls and emails. An in-house coder will typically have
completed the necessary courses and will be able to perform routine
administrative tasks such as scheduling appointments, receiving and entering
information on patients, submitting medical diagnosis codes, filing insurance
claims, sending billing and claim requests to health insurers and health plans,
and handling routine correspondence from patients and health insurance
companies.
It is
important for health care providers to understand the differences between
medical billing and medical coding. Medical billing usually refers to the
process by which health care providers submit claims to insurance companies for
payment. Medical coding, on the other hand, refers to the method of assigning
codes to various medical diagnoses and procedures so that these can be used by
a doctor, nurse, or other medical professional for billing. In order to
accurately assign appropriate codes to different medical diagnoses and
procedures, a qualified professional must be properly trained. Medical billing
usually involves more paper-based processes than does medical coding.
Both
processes involve the use of current procedural terminology (CPT) codes. Health
care providers should check with their health plan administrator to ensure they
are correctly using CPT codes when they file claims. Medical billing and coding
professionals are certified in CPT and HIPAA codes. They are required to take a
comprehensive training course in both coding and billing before working professionally.
Post Your Ad Here
Comments