How to Advance Towards Achieving 100% Interoperability in Healthcare?
by Pawan Yadav ManagerInteroperability can be dubbed as a data superhighway, but the majority of healthcare stakeholders are still stuck in a parking lot. Integrating and utilizing EHRs together are the first baby steps. Healthcare Interoperability will be an ongoing challenge for healthcare stakeholders due to the industry’s unique information exchange requirements and stringent compliance mandates. If we aim to overcome these hurdles, then achieving 100% EHR interoperability is the final summit where we are yet to reach.
Data Belongs to the Patients

“The idea that patient data belongs to providers or vendors is an epic misunderstanding. Patient data belongs to patients” –Seema Verma, Administrator CMS
CMS released proposed rules that require many types of insurers to provide electronic health data in a standard format by 2020. These rules require healthcare providers and health plans to implement open data-sharing systems to ensure data can easily flow from one system to another, potentially by way of patient apps.
The major goal of CMS and the Office of the National Coordinator for Health Information Technology is to empower patients to control their own healthcare data and finally put them in the driver’s seat. The healthcare industry now needs to rely on modern technology, such as the near-ubiquitous use of smartphones and mobile apps to allow patients to take command of their care by virtue of gaining further access to their data.
How Interoperability Exists Today
Various interoperability standards such as Health Level Seven (HL7) and FHIR are competent in the industry for better streamlining of health documentation and care coordination. With the help of FHIR, doctors can get access to the health data on their mobile phones through multiple API functions that FHIR supports. Ability to access accurate data from sources other than EHRs is the need of the hour.
The Curious Case of Health Data Exchange
Since1987, HL7 International has been working on healthcare data standards to create and improve the standards in use throughout the healthcare industry.
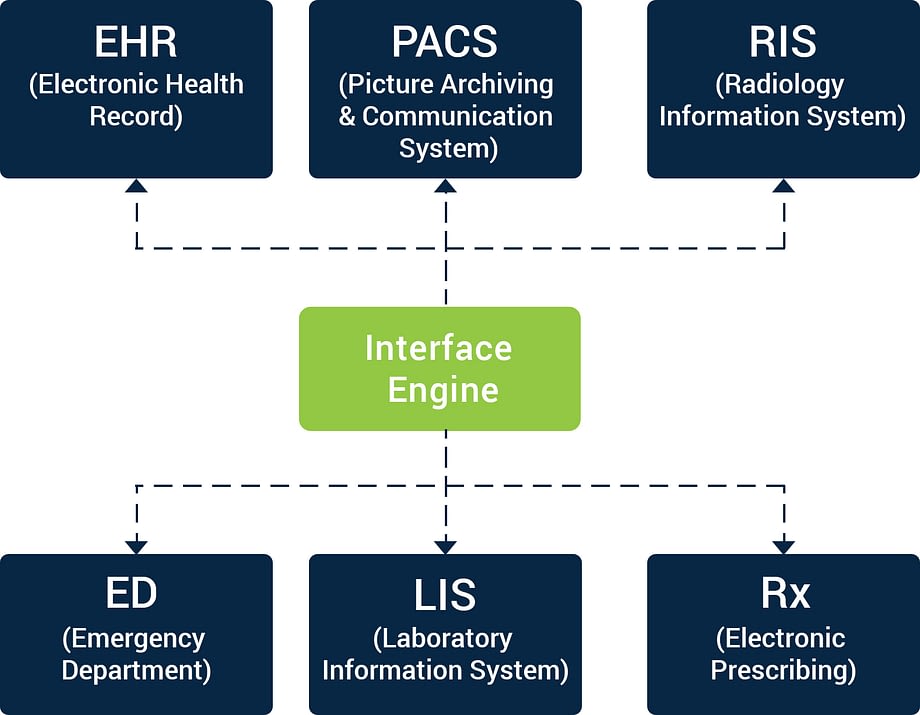
Different systems have varied workflows which are supposed to work well in a patient facility or an ambulatory environment. The technology leveraged should be flexible and easily configurable. The traditional data exchange pattern should be replaced with data exchange through an advanced integration engine.
Integration engines can act as a hub to offer seamless integration and cut down the development cost and time drastically. Integration engines are quick and simplify the workflow for central monitoring, flow control, alerting, data mapping, and more, to organize the data flow within these applications.
The Story Behind Healthcare APIs
The healthcare industry cannot optimize interoperability without creating data and adhering to data standards. The healthcare industry needs to adopt a standardized implementation model with the help of web APIs.

APIs are also being deployed within business intelligence platforms to create a centralized, 360-degree view of the patient. They represent a framework for solving complex clinical problems. The true IoT experience can be made possible with APIs where people can push the data from their medical devices directly to the medical records with ease. Multiple data sources such as genomics and lab data will be transferable. As APIs are helping these providers to offer more precise care based on all the data being accumulated from APIs coming in from apps and hardware.
SMART on FHIR
Developed by Boston Children’s Hospital and Harvard Medical School Department of Biomedical Informatics in 2010, and SMART on FHIR is immensely supported by the healthcare industry. It focuses on three key areas.
Sponsor Ads
Created on Sep 17th 2019 06:05. Viewed 372 times.



